Knee Osteoarthritis – Prevention, Treatment & Management

Have you ever suffered from knee pain? One of the most common causes of knee pain is knee osteoarthritis. Did you know that about 10% of all men and 13% of all women over the age of 60 have symptomatic knee osteoarthritis? Of those individuals, about 80% have limitation in their activities of daily living from their symptoms. Did you also know that knee osteoarthritis is one of the leading causes for disability for the older adult which leads to significant health care expenditure? Osteoarthritis is often referred to as degenerative joint disease, and commonly affects high load bearing joints such as the knees.
Luckily for individuals suffering from knee pain related to arthritic changes at the knee, there are many viable treatment options. Because of the high prevalence of knee arthritis, there is now extensive research on identifying risk factors and effectiveness of treatment to reduce limitations and disability associated with this pathology. In this post, we will briefly discuss how you can reduce osteoarthritis risk factors and manage this condition.
What Is Knee Osteoarthritis?
Osteo = Bone
Arthro = Joint
Itis = Inflammation
Knee osteoarthritis is a degenerative process that occurs when the cartilage layer on the end of two articulating bones begins to wear down allowing for those bone to come into direct contact with one another. You may have heard some medical providers describe this to you as “bone-on-bone”. This often leads to pain and osteophyte (bone spur) formation, which compounds this disease.
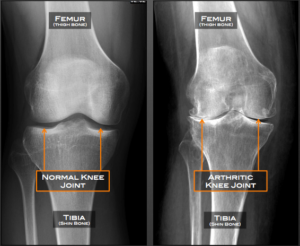
For the example of the knee, this means that the articular cartilage layer between the tibia (shin bone) and the femur (thigh bone) has worn down. The cartilage that has been damaged has an extremely low capacity to regenerate itself. If not properly addressed, this progressive degeneration can continue over time. Pain, morning stiffness, decreased range of motion, bony enlargement, inflammation, crepitus, and decreased function are some of the symptoms associated with osteoarthritis. Osteoarthritis can occur in joints throughout the body, however it is most common in the knees and hips.
Risk Factors For Knee Osteoarthritis
There are many factors that play a role in the development of osteoarthritis and are related to modifiable and non-modifiable risk factors. There has been significant literature that shows a genetic component to the development of this disease. However, many of the risk factors are things we can modify in our daily lives. A research study that performed a systematic review of scientific evidence relating to osteoarthritis has been able to identify several risk factors. They are as follows:
- Older Age
- As a result of the degenerative process of this disease, higher incidences of osteoarthritis are seen as we age
- The cumulative forces that our joints undergo through life will eventually cause some mild degenerative changes
- Nutrition
- There are implications to vitamin C, D and development of osteoarthritis
- We still have a lot to learn about how nutrition affects the development of certain conditions and diseases
- Gender
- Females are more likely to get osteoarthritis which may be related to hormones and other factors
- Females also tend to have wider hips, creating an inward angle at the hips that can lead to increased joint stress on the inside of the knee
- Obesity
- This is often difficult to address with patients, but makes perfect sense. More weight through the joint = more stress to the joint
- To greater the degree of overweightness or obesity has stronger correlation with incidence of knee osteoarthritis
- Previous Knee Injury
- Such as meniscus tear
- The risk is much higher when you’ve had a previous knee surgery
- Repetitive Trauma / Mechanical Forces
- This is an interesting argument. A study to determine the incidence of arthritis in runners (which can be categorized as repetitive trauma or impact) compared to the sedentary population showed that recreational runners have a 3.5% risk of development, while the sedentary population had approximately a 10.2% risk and competitive runners had a 13.3% risk. From a surface level evaluation, there seems to be an activity threshold at which the body can withstand repetitive impact and even adapt to improve its ability to take that load, but too great of a stimulus or volume may lead to detrimental effects on the joint surface.
- Muscle Weakness
- Stronger muscles can help absorb weight-bearing forces and take stress off the joint
- Weakness specifically relating to the quadriceps muscle is a risk factor for knee osteoarthritis
- Joint Laxity
- Which is often due to congenital differences in tissue composition or decreased muscle tone
- Joint Deformity
- Anatomical or injury related differences in joint surfaces
How to Manage Osteoarthritis
So now your question is probably, “If this process has begun how can I manage it?” Management of this disease can be generally broken down into two categories: conservative and surgical.
Conservative treatment generally implies the combination of pharmaceutical therapy (non-steroidal anti-inflammatory drugs, pain relieving pharmaceuticals, or other oral supplements such as glucosamine and chondroitin sulfate), intra articular corticosteroid injection, physical therapy, and activity modification. Other newer treatments show some signs of promise such as platelet rich plasma injections or stem cell treatment for management of symptoms and progression of disease.
One of the BEST things you can do to both prevent and manage knee osteoarthritis is exercise. As mentioned above, there is clearly a strong correlation between exercise and joint health. Exercise, weight-bearing force, and movement help bring nutrients into the joint and aid in the removal of waste products. Building up strength around the joint also helps to reduce joint forces. As the muscles get stronger, they can absorb for of the forces, thus taking stress away from the joint itself.
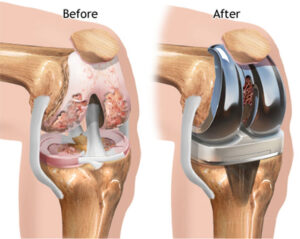
Surgical treatment is usually saved for when conservative treatments have been exhausted and the patient’s symptoms severely limit their function. The most typical and best surgical treatment is currently a total joint arthroplasty, or total joint replacement. In this procedure, the arthritic surfaces of the articulating joint are replaced with artificial materials. Outcomes of total knee replacement are very good, and increasingly better when individuals combine surgery with post-operative physical therapy rehab. If you are contemplating this type of procedure, be sure to come in and get a physical therapy evaluation prior to the procedure so that you can start on rehab exercises immediately after surgery. The quicker you start physical therapy, the better your outcomes will be.
How Can Your Doctor of Physical Therapy Help with Knee Osteoarthritis?
As physical therapists, we can evaluate joint kinematics, muscle imbalances, strength deficits, muscle length issues, aggravating activities, and dysfunctional movement patterns which may be contributing to your pain and symptoms. We can also assist with structured and supervised treatment plans to reach optimal function. There is ample research to support the use of physical therapy as conservative treatment as well as therapy pre AND post-surgery for osteoarthritis to improve patient outcomes. If you are contemplating treatment plans to combat progressing knee osteoarthritis, come check us out and we can get you started on a return to doing the things that you love to do!
If you want to read more, I suggest checking out this article: http://annals.org/aim/fullarticle/713937/osteoarthritis-new-insights-part-1-disease-its-risk-factors
As always feel free to comment below and ask questions as needed!


